Colorectal Cancer
What are colon and rectum?
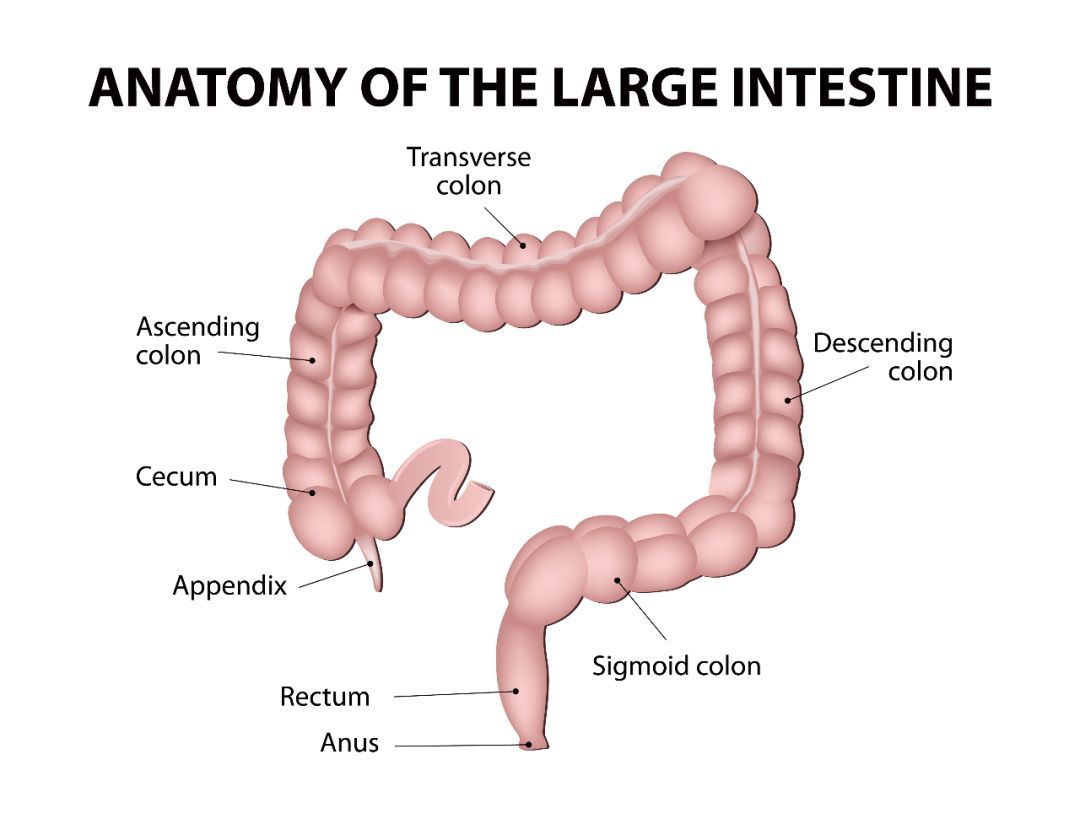
Colon and rectum are the parts of large intestine, which is the lowest part of the digestive system. Colon is about 5 feet long and absorbs water from stool.
Rectum is the last 12 centimeters (nearly 5 inches) of the colon, where the body stores stools until you have a bowel movement.
What is colorectal cancer?
Colorectal cancer is the cancer of the colon and/or rectum which begins with the development of pre-cancerous polyps from the lining of the colon and rectum. These cancers can also be named colon cancer or rectal cancer, depending on where they start.
Colon cancer typically affects older adults, though it can happen at any age. It usually begins as small, noncancerous (benign) clumps of cells called polyps that form on the inside of the colon. Over time some of these polyps can become colon cancer.
If colon cancer develops, many treatments are available to help control it, including surgery, radiation therapy and drug treatments, such as chemotherapy, targeted therapy and immunotherapy.
Risk factors
| Non modifiable | Modifiable |
| Age | Obesity |
| Personal history of colorectal polyps or colorectal cancer | Smoking |
| A personal history of inflammatory bowel disease (IBD) | Type II Diabetes |
| Family history of colorectal cancer | Alcohol |
| Race or ethnic background | Sedentary life style |
| Inherited syndromes that increase colon cancer risk | Certain types of diets - diet rich in red meats and processed meats |
| Radiation therapy for cancer |
When should you consult a doctor? What are the early signs and symptoms?
- Changes in bowel habits, including persistent constipation or diarrhea, a feeling of not being able to empty the bowel completely, an urgency to move the bowels, or a change in the consistency of the stools (long, thin “pencil stools”)
- Rectal bleeding or dark patches of blood in or on stool
- Persistent abdominal discomfort such as cramps, bloating, gas or pain
- Unexplained fatigue, weakness, loss of appetite and/or weight loss
- Pelvic pain, which occurs at later stages of the disease
- Most people with colorectal cancer do not experience any symptoms or have only non-specific symptoms in the early stages. When the symptoms appear, they vary depending upon the size and location of tumor in the intestine.
- Few patients with right colon tumors present with anaemia and generalized weakness
- Left colon and rectal cancers can present with emergency symptoms of bowel obstruction
How can it be diagnosed?
Its imperative to visit a GI surgical oncologist at the earliest symptom or sign suggestive of colorectal cancer.
- History & Physical Examination: Complete medical history for presence of risk factors, including your family history and digital rectal examination (DRE) may also be performed. In this test, a gloved and lubricated finger is inserted into the rectum to feel for any abnormal areas.
- Blood tests: Hemogram and Liver enzymes
- Serum tumor markers: For colorectal cancer, the most common tumor markers tested include Carcinoembryonic antigen (CEA) and CA 19-9.
- Colonoscopy: This is the most commonly used test to diagnose colorectal cancer if the symptoms are highly suggestive. It allows the doctor to look at the entire length of the colon and rectum using a colonoscope which is a thin flexible lighted tube with camera at the end attached to a monitor on the doctor’s desk.
- Biopsy: Tissue biopsy is taken during colonoscopy from any suspicious area and the sample is sent to pathology lab for testing by a pathologist who looks for cancer cells in the specimen. Genetic tests may also be done on the biopsy specimens to identify specific gene changes in the cancer cells. These tests are available at very few centres in the country.
- Imaging Tests:
- 1. Computed tomography (CT) scan of the chest and abdomen - can help to find out if the colorectal cancer has spread to liver and other organs.
- 2. Ultrasound: Endorectal USG, in which a special transducer is inserted into the rectum, can help to see how far the cancer has penetrated the rectal wall.
- 3. Magnetic resonance imaging (MRI) can help to look for local spread of colorectal cancer so that treatment can be planned accordingly.
- 4. PETCT – may be performed in select patients according the pathology of tumor and results of CT or MRI
Treatment of Colorectal cancer
Different modalities to treat colorectal cancer include:
- Surgery – remains the curative modality for patients with localized, locally advanced and oligometastatic (single site liver/lung metastases) cancer.
- Radiotherapy – Is advised for all locally advanced rectal cancers before surgery. Radiotherapy can be administered along with chemotherapy for better effect.
- Chemotherapy – Plays a role in adjuvant treatment (after surgery) and for patients with metastatic disease.
- Targeted therapy – Is used for metastatic cancer
These are used alone or in combination depending on the stage of the cancer, performance status of the patient, grade of the tumor and other factors.
Surgery for colon cancer
Surgery currently is the definitive treatment modality. The type of surgery used depends on the stage (extent) of the cancer, where it is, and the goal of the surgery.
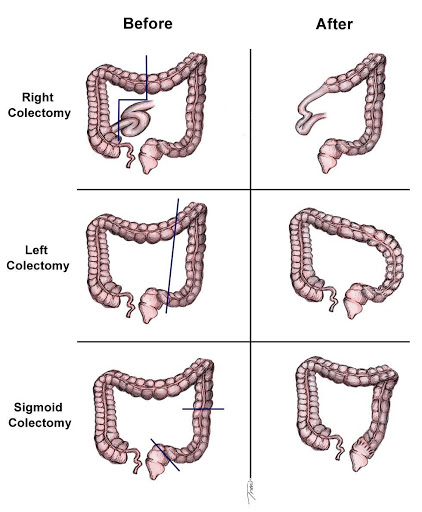
Colectomy - A colectomy is surgery to remove all or part of the colon along with adjacent lymph nodes. Complete mesocolic excision should be done for better results.
How it's done?
A colectomy can be done in 2 ways:
Open colectomy: The surgery is done through a single long incision (cut) in the abdomen (belly).
Laparoscopic-assisted colectomy: The surgery is done through many smaller incisions and special tools.
Surgery for Rectal Cancer
Surgery is usually the main treatment for rectal cancer. Radiation and chemotherapy are often given before or after surgery. The type of surgery used depends on the stage (extent) of the cancer, where it is, how close the tumor is to the anus and if it has spread to the ring like sphincter ,uscles around the anus.
Local transanal resection (full thickness resection)
This procedure can be used to remove some early stage I rectal cancers that are relatively small and not too far from the anus. Local transanal resection (also known as transanal excision) is done with instruments that are put into the rectum through the anus.
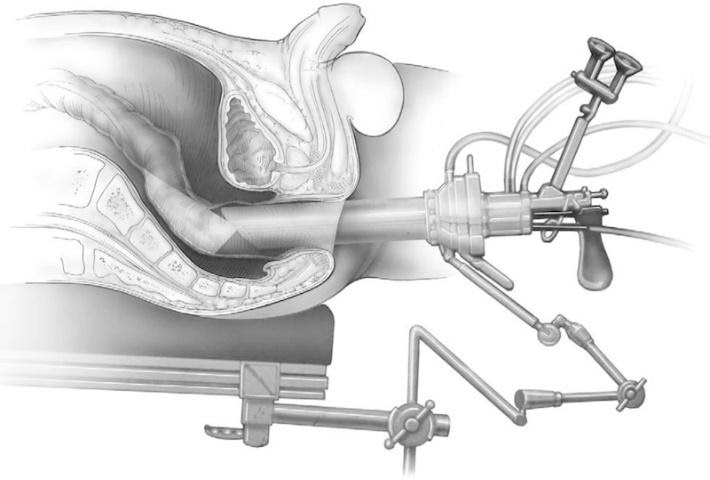
Transanal endoscopic microsurgery (TEM)
This operation can sometimes be used for early stage I cancers that are higher in the rectum and can't be reached using the standard transanal resection. A specially designed magnifying scope is put through the anus and into the rectum. This allows the surgeon to do a transanal resection with great precision and accuracy. This operation requires special equipment and surgeons with special training and experience, so it's only done at certain cancer centers.
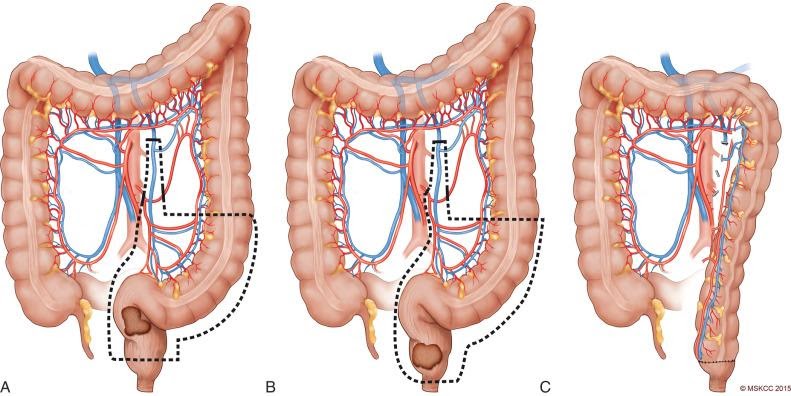
Low anterior resection (LAR)
Some stage I rectal cancers and most stage II or III cancers in the upper part of the rectum (close to where it connects with the colon) can be removed by low anterior resection (LAR). In this operation, the part of the rectum containing the tumor is removed. The colon is then attached to the remaining part of the rectum (either right away or sometime later) so that the patient moves their bowels in the usual way.
If radiation and chemotherapy have been given before surgery, it's common for a short-term ileostomy to be made. (This is where the end of the ileum, the last part of the small intestine, is connected to a hole in the skin of the abdomen.) This gives the rectum time to heal before body waste moves through it again. In most cases, the ileostomy can be reversed (the intestines are reconnected) about 8 weeks later.
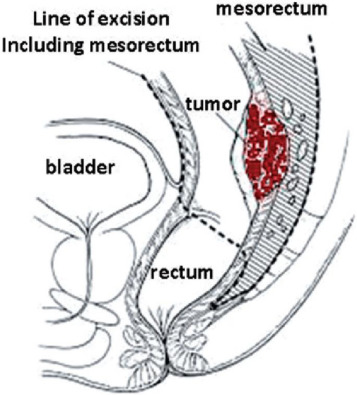
Total mesorectal excision (TME)
TME (which can be defined as complete excision of visceral mesorectum to the level of the levator, with the preservation of the pelvic nerves) is the gold standard for the treatment of rectal cancers and the middle lower third of the rectum. It is performed for all upper and mid rectal cancers.
Proctectomy with colo-anal anastomosis
Some stage I and most stage II and III rectal cancers in the middle and lower third of the rectum require removing the entire rectum (called a proctectomy). The rectum has to be removed so that a total mesorectal excision (TME) can be done to remove all of the lymph nodes near the rectum. The colon is then connected to the anus (called a colo-anal anastomosis) so that the patient will move their bowels in the usual way.
Intersphincteric resection
For patients with partial involvement of anal sphincter by rectal tumor, intersphincteric resection is offered and colon is connected to anus (colo-anal anastomoses).
Abdominoperineal resection (APR)
It's often needed if the cancer is growing into the sphincter muscle (the muscle that keeps the anus closed and prevents stool leakage) or the nearby muscles that help control urine flow (called levator muscles). Both the rectum and anal canal are removed. Because the anus is removed, a permanent colostomy is created (the end of the colon is connected to a hole in the skin over the abdomen) to allow stool to leave the body.
Pelvic exenteration
If the rectal cancer is growing into nearby organs, a pelvic exenteration may be recommended. This is major operation. The surgeon will remove the rectum as well as any nearby organs that the cancer has reached, such as the bladder, prostate (in men), or uterus (in women). A colostomy is needed after pelvic exenteration. If the bladder is removed, a urostomy is needed, too.
Diverting colostomy
Some patients have rectal cancers that have spread and also have tumors blocking the rectum. In this case, surgery may be done to relieve the blockage without removing the part of the rectum containing the cancer. Instead, the colon is cut above the tumor and attached to a stoma (an opening in the skin of the abdomen) to allow stool to come out. This is called a diverting colostomy. It can often help the patient recover enough to start other treatments (such as chemotherapy).
